
Ai In Healthcare Revenue Cycle Management Market
AI in Healthcare Revenue Cycle Management Market Forecasts to 2034 - Global Analysis By Component (Software and Services), Solution Type, Deployment Mode, Technology, Application, End User and By Geography

According to Stratistics MRC, the Global AI in Healthcare Revenue Cycle Management Market is accounted for $4.9 billion in 2026 and is expected to reach $38.5 billion by 2034, growing at a CAGR of 29.4% during the forecast period. AI in Healthcare Revenue Cycle Management involves using intelligent algorithms and machine learning to enhance the efficiency of healthcare financial operations. It automates processes like billing, claims handling, payment tracking, and managing claim denials, minimizing errors and saving time. By examining extensive healthcare data, AI detects inconsistencies, predicts revenue losses, and supports better decision-making, thereby improving operational workflows, lowering costs, and strengthening the financial health of medical institutions.
Market Dynamics:
Driver:
Need for operational efficiency and cost reduction
Healthcare organizations are under immense pressure to reduce administrative costs while managing complex billing processes. Traditional RCM systems are often plagued by manual errors, claim denials, and slow reimbursement cycles, leading to significant revenue leakage. AI-driven automation addresses these challenges by streamlining workflows, automating repetitive tasks like prior authorizations and coding, and accelerating claims processing. By reducing the administrative burden on staff and minimizing costly errors, AI solutions enable providers to improve cash flow and allocate resources more effectively. This growing need for financial optimization and operational agility is a primary driver accelerating the adoption of AI in RCM.
Restraint:
High implementation costs and integration complexities
The initial investment required for AI-powered RCM solutions, including software procurement, infrastructure upgrades, and staff training, can be prohibitive, particularly for small and mid-sized healthcare providers. Furthermore, integrating AI platforms with legacy hospital information systems and electronic health records (EHRs) presents significant technical challenges. Data silos, interoperability issues, and the need for extensive data cleansing to ensure algorithm accuracy add to the complexity and cost. These financial and technical barriers can slow down the rate of adoption, making it difficult for organizations with limited IT budgets and resources to transition from traditional RCM processes.
Opportunity:
Advancements in generative AI and predictive analytics
The emergence of generative AI and sophisticated predictive analytics is unlocking new frontiers in RCM. Generative AI can automate complex tasks such as drafting appeal letters for denied claims and generating clinical documentation summaries. Predictive analytics models can forecast claim denials before submission, allowing for pre-emptive corrections, and accurately predict payment timelines. These advanced capabilities not only enhance revenue capture but also provide strategic financial insights. As these technologies mature and become more accessible, they offer significant opportunities for solution providers to develop more intelligent, autonomous RCM systems that deliver higher ROI for healthcare organizations.
Threat:
Data privacy and security concerns
The healthcare sector is a prime target for cyberattacks, and AI systems that process vast amounts of sensitive patient financial and clinical data present a significant security risk. Compliance with stringent regulations like HIPAA in the U.S. and GDPR in Europe is mandatory, and any data breach can result in severe financial penalties and reputational damage. The use of AI also introduces complexities regarding data governance and algorithmic bias. Concerns about patient data confidentiality and the potential for security vulnerabilities in AI models can create hesitation among healthcare providers, potentially hindering the widespread adoption of cloud-based and integrated AI RCM solutions.
Covid-19 Impact
The COVID-19 pandemic severely disrupted healthcare finances, with a sharp decline in elective procedures and a surge in operational costs, highlighting the fragility of traditional RCM systems. The crisis accelerated the shift towards digital transformation, compelling providers to adopt AI and automation to manage surging claims volumes, patient inquiries, and remote billing operations. The need for touchless, efficient processes became paramount. Post-pandemic, healthcare organizations are prioritizing resilient, AI-driven RCM infrastructure to handle fluctuating patient volumes, ensure financial stability, and adapt to evolving care delivery models like telehealth, making AI a strategic necessity rather than a technological luxury.
The claims management & claims scrubbing segment is expected to be the largest during the forecast period
The claims management & claims scrubbing segment is expected to hold the largest market share, driven by the critical need to minimize claim denials and accelerate reimbursements. These AI solutions automatically detect coding errors, verify payer-specific rules, and correct claims before submission, significantly reducing rejection rates. As reimbursement models become more complex and payer requirements more stringent, healthcare providers are heavily investing in AI to safeguard revenue integrity. The segment’s dominance is reinforced by its direct impact on financial performance, offering a clear return on investment by streamlining the most financially sensitive step in the revenue cycle.
The ambulatory surgical centers (ASCs) segment is expected to have the highest CAGR during the forecast period
Over the forecast period, the ambulatory surgical centers (ASCs) segment is anticipated to witness the highest growth rate. ASCs are increasingly adopting AI to manage the unique financial complexities of high-volume, outpatient procedures. With limited administrative staff, these centers rely on AI for efficient patient eligibility verification, automated coding, and rapid claims processing to maintain profitability. The shift of surgical procedures from hospitals to ASCs, coupled with a focus on operational efficiency, is fueling this demand. AI enables ASCs to optimize their lean business models, ensuring faster payment cycles and improved financial viability.
Region with largest share:
During the forecast period, the North America region is expected to hold the largest market share, attributed to the presence of a highly advanced healthcare IT infrastructure and early adoption of cutting-edge technologies. Stringent regulatory requirements for billing compliance and the need to reduce high administrative costs are driving significant investment. The region’s concentrated presence of major AI and healthcare technology vendors further accelerates market growth, supported by favorable reimbursement landscapes that encourage digital transformation.
Region with highest CAGR:
Over the forecast period, the Asia Pacific region is anticipated to exhibit the highest CAGR, fueled by rapid digitalization of healthcare systems and increasing healthcare expenditure. Countries like China, India, and Japan are witnessing a surge in hospital infrastructure projects and government initiatives promoting healthcare efficiency. The growing medical tourism industry and the need to manage large patient populations cost-effectively are driving the adoption of AI-driven RCM solutions to enhance operational productivity and financial accuracy.
Key players in the market
Some of the key players in AI in Healthcare Revenue Cycle Management Market include R1 RCM Inc., Experian Health, athenahealth, McKesson Corporation, Oracle Health, eClinicalWorks, CareCloud, Infinx, XiFin Inc., VisiQuate, Thoughtful AI, Adonis, Zentist, Firstsource, and RapidClaims.
Key Developments:
In January 2025, R1 RCM Inc. launched a new generative AI platform designed to automate patient-physician interactions and streamline prior authorization workflows. The platform leverages large language models to reduce manual effort, significantly cutting down the time required to secure insurance approvals and improving the overall patient financial experience.
In November 2024, Athenahealth announced a new set of AI-powered capabilities within its network, designed to automate clinical documentation and medical coding. This integration aims to reduce administrative burden for physicians and accelerate the revenue cycle by enabling faster and more accurate charge capture directly from patient encounters.
Components Covered:
• Software
• Services
Solution Types Covered:
• Integrated AI RCM Solutions
• Standalone AI Solutions
Deployment Modes Covered:
• Cloud-Based Solutions
• Web-Based Solutions
• On-Premise Solutions
Technologies Covered:
• Machine Learning (ML)
• Natural Language Processing (NLP)
• Robotic Process Automation (RPA)
• Predictive Analytics
• Generative AI
Applications Covered:
• Patient Access & Eligibility Verification
• Medical Coding Automation
• Claims Management & Claims Scrubbing
• Denial Management
• Charge Capture
• Billing & Payment Processing
• Payment Posting
• Revenue Forecasting & Financial Analytics
• Clinical Documentation Improvement (CDI)
• Accounts Receivable (AR) Management
End Users Covered:
• Hospitals
• Physician Back Offices
• Diagnostic Laboratories
• Ambulatory Surgical Centers (ASCs)
• Healthcare Payers
• Other End Users
Regions Covered:
• North America
o United States
o Canada
o Mexico
• Europe
o United Kingdom
o Germany
o France
o Italy
o Spain
o Netherlands
o Belgium
o Sweden
o Switzerland
o Poland
o Rest of Europe
• Asia Pacific
o China
o Japan
o India
o South Korea
o Australia
o Indonesia
o Thailand
o Malaysia
o Singapore
o Vietnam
o Rest of Asia Pacific
• South America
o Brazil
o Argentina
o Colombia
o Chile
o Peru
o Rest of South America
• Rest of the World (RoW)
o Middle East
§ Saudi Arabia
§ United Arab Emirates
§ Qatar
§ Israel
§ Rest of Middle East
o Africa
§ South Africa
§ Egypt
§ Morocco
§ Rest of Africa
What our report offers:
- Market share assessments for the regional and country-level segments
- Strategic recommendations for the new entrants
- Covers Market data for the years 2023, 2024, 2025, 2026, 2027, 2028, 2030, 2032 and 2034
- Market Trends (Drivers, Constraints, Opportunities, Threats, Challenges, Investment Opportunities, and recommendations)
- Strategic recommendations in key business segments based on the market estimations
- Competitive landscaping mapping the key common trends
- Company profiling with detailed strategies, financials, and recent developments
- Supply chain trends mapping the latest technological advancements
Free Customization Offerings:
All the customers of this report will be entitled to receive one of the following free customization options:
• Company Profiling
o Comprehensive profiling of additional market players (up to 3)
o SWOT Analysis of key players (up to 3)
• Regional Segmentation
o Market estimations, Forecasts and CAGR of any prominent country as per the client's interest (Note: Depends on feasibility check)
• Competitive Benchmarking
o Benchmarking of key players based on product portfolio, geographical presence, and strategic alliances
Table of Contents
1 Executive Summary
1.1 Market Snapshot and Key Highlights
1.2 Growth Drivers, Challenges, and Opportunities
1.3 Competitive Landscape Overview
1.4 Strategic Insights and Recommendations
2 Research Framework
2.1 Study Objectives and Scope
2.2 Stakeholder Analysis
2.3 Research Assumptions and Limitations
2.4 Research Methodology
2.4.1 Data Collection (Primary and Secondary)
2.4.2 Data Modeling and Estimation Techniques
2.4.3 Data Validation and Triangulation
2.4.4 Analytical and Forecasting Approach
3 Market Dynamics and Trend Analysis
3.1 Market Definition and Structure
3.2 Key Market Drivers
3.3 Market Restraints and Challenges
3.4 Growth Opportunities and Investment Hotspots
3.5 Industry Threats and Risk Assessment
3.6 Technology and Innovation Landscape
3.7 Emerging and High-Growth Markets
3.8 Regulatory and Policy Environment
3.9 Impact of COVID-19 and Recovery Outlook
4 Competitive and Strategic Assessment
4.1 Porter's Five Forces Analysis
4.1.1 Supplier Bargaining Power
4.1.2 Buyer Bargaining Power
4.1.3 Threat of Substitutes
4.1.4 Threat of New Entrants
4.1.5 Competitive Rivalry
4.2 Market Share Analysis of Key Players
4.3 Product Benchmarking and Performance Comparison
5 Global AI in Healthcare Revenue Cycle Management Market, By Component
5.1 Software
5.1.1 AI-based RCM Platforms
5.1.2 Predictive Analytics & AI Algorithms
5.1.3 Automation & Workflow Management Tools
5.2 Services
5.2.1 Consulting Services
5.2.2 Implementation & Integration
5.2.3 Training & Support
5.2.4 Managed RCM Services
6 Global AI in Healthcare Revenue Cycle Management Market, By Solution Type
6.1 Integrated AI RCM Solutions
6.2 Standalone AI Solutions
7 Global AI in Healthcare Revenue Cycle Management Market, By Deployment Mode
7.1 Cloud-Based Solutions
7.2 Web-Based Solutions
7.3 On-Premise Solutions
8 Global AI in Healthcare Revenue Cycle Management Market, By Technology
8.1 Machine Learning (ML)
8.2 Natural Language Processing (NLP)
8.3 Robotic Process Automation (RPA)
8.4 Predictive Analytics
8.5 Generative AI
9 Global AI in Healthcare Revenue Cycle Management Market, By Application
9.1 Patient Access & Eligibility Verification
9.2 Medical Coding Automation
9.3 Claims Management & Claims Scrubbing
9.4 Denial Management
9.5 Charge Capture
9.6 Billing & Payment Processing
9.7 Payment Posting
9.8 Revenue Forecasting & Financial Analytics
9.9 Clinical Documentation Improvement (CDI)
9.10 Accounts Receivable (AR) Management
10 Global AI in Healthcare Revenue Cycle Management Market, By End User
10.1 Hospitals
10.2 Physician Back Offices
10.3 Diagnostic Laboratories
10.4 Ambulatory Surgical Centers (ASCs)
10.5 Healthcare Payers
10.6 Other End Users
11 Global AI in Healthcare Revenue Cycle Management Market, By Geography
11.1 North America
11.1.1 United States
11.1.2 Canada
11.1.3 Mexico
11.2 Europe
11.2.1 United Kingdom
11.2.2 Germany
11.2.3 France
11.2.4 Italy
11.2.5 Spain
11.2.6 Netherlands
11.2.7 Belgium
11.2.8 Sweden
11.2.9 Switzerland
11.2.10 Poland
11.2.11 Rest of Europe
11.3 Asia Pacific
11.3.1 China
11.3.2 Japan
11.3.3 India
11.3.4 South Korea
11.3.5 Australia
11.3.6 Indonesia
11.3.7 Thailand
11.3.8 Malaysia
11.3.9 Singapore
11.3.10 Vietnam
11.3.11 Rest of Asia Pacific
11.4 South America
11.4.1 Brazil
11.4.2 Argentina
11.4.3 Colombia
11.4.4 Chile
11.4.5 Peru
11.4.6 Rest of South America
11.5 Rest of the World (RoW)
11.5.1 Middle East
11.5.1.1 Saudi Arabia
11.5.1.2 United Arab Emirates
11.5.1.3 Qatar
11.5.1.4 Israel
11.5.1.5 Rest of Middle East
11.5.2 Africa
11.5.2.1 South Africa
11.5.2.2 Egypt
11.5.2.3 Morocco
11.5.2.4 Rest of Africa
12 Strategic Market Intelligence
12.1 Industry Value Network and Supply Chain Assessment
12.2 White-Space and Opportunity Mapping
12.3 Product Evolution and Market Life Cycle Analysis
12.4 Channel, Distributor, and Go-to-Market Assessment
13 Industry Developments and Strategic Initiatives
13.1 Mergers and Acquisitions
13.2 Partnerships, Alliances, and Joint Ventures
13.3 New Product Launches and Certifications
13.4 Capacity Expansion and Investments
13.5 Other Strategic Initiatives
14 Company Profiles
14.1 R1 RCM Inc.
14.2 Experian Health
14.3 athenahealth
14.4 McKesson Corporation
14.5 Oracle Health
14.6 eClinicalWorks
14.7 CareCloud
14.8 Infinx
14.9 XiFin Inc.
14.10 VisiQuate
14.11 Thoughtful AI
14.12 Adonis
14.13 Zentist
14.14 Firstsource
14.15 RapidClaims
List of Tables
1 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Region (2023-2034) ($MN)
2 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Component (2023-2034) ($MN)
3 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Software (2023-2034) ($MN)
4 Global AI in Healthcare Revenue Cycle Management Market Outlook, By AI-based RCM Platforms (2023-2034) ($MN)
5 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Predictive Analytics & AI Algorithms (2023-2034) ($MN)
6 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Automation & Workflow Management Tools (2023-2034) ($MN)
7 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Services (2023-2034) ($MN)
8 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Consulting Services (2023-2034) ($MN)
9 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Implementation & Integration (2023-2034) ($MN)
10 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Training & Support (2023-2034) ($MN)
11 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Managed RCM Services (2023-2034) ($MN)
12 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Solution Type (2023-2034) ($MN)
13 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Integrated AI RCM Solutions (2023-2034) ($MN)
14 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Standalone AI Solutions (2023-2034) ($MN)
15 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Deployment Mode (2023-2034) ($MN)
16 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Cloud-Based Solutions (2023-2034) ($MN)
17 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Web-Based Solutions (2023-2034) ($MN)
18 Global AI in Healthcare Revenue Cycle Management Market Outlook, By On-Premise Solutions (2023-2034) ($MN)
19 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Technology (2023-2034) ($MN)
20 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Machine Learning (ML) (2023-2034) ($MN)
21 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Natural Language Processing (NLP) (2023-2034) ($MN)
22 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Robotic Process Automation (RPA) (2023-2034) ($MN)
23 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Predictive Analytics (2023-2034) ($MN)
24 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Generative AI (2023-2034) ($MN)
25 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Application (2023-2034) ($MN)
26 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Patient Access & Eligibility Verification (2023-2034) ($MN)
27 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Medical Coding Automation (2023-2034) ($MN)
28 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Claims Management & Claims Scrubbing (2023-2034) ($MN)
29 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Denial Management (2023-2034) ($MN)
30 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Charge Capture (2023-2034) ($MN)
31 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Billing & Payment Processing (2023-2034) ($MN)
32 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Payment Posting (2023-2034) ($MN)
33 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Revenue Forecasting & Financial Analytics (2023-2034) ($MN)
34 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Clinical Documentation Improvement (CDI) (2023-2034) ($MN)
35 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Accounts Receivable (AR) Management (2023-2034) ($MN)
36 Global AI in Healthcare Revenue Cycle Management Market Outlook, By End User (2023-2034) ($MN)
37 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Hospitals (2023-2034) ($MN)
38 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Physician Back Offices (2023-2034) ($MN)
39 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Diagnostic Laboratories (2023-2034) ($MN)
40 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Ambulatory Surgical Centers (ASCs) (2023-2034) ($MN)
41 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Healthcare Payers (2023-2034) ($MN)
42 Global AI in Healthcare Revenue Cycle Management Market Outlook, By Other End Users (2023-2034) ($MN)
Note: Tables for North America, Europe, APAC, South America, and Rest of the World (RoW) are also represented in the same manner as above.
List of Figures
RESEARCH METHODOLOGY
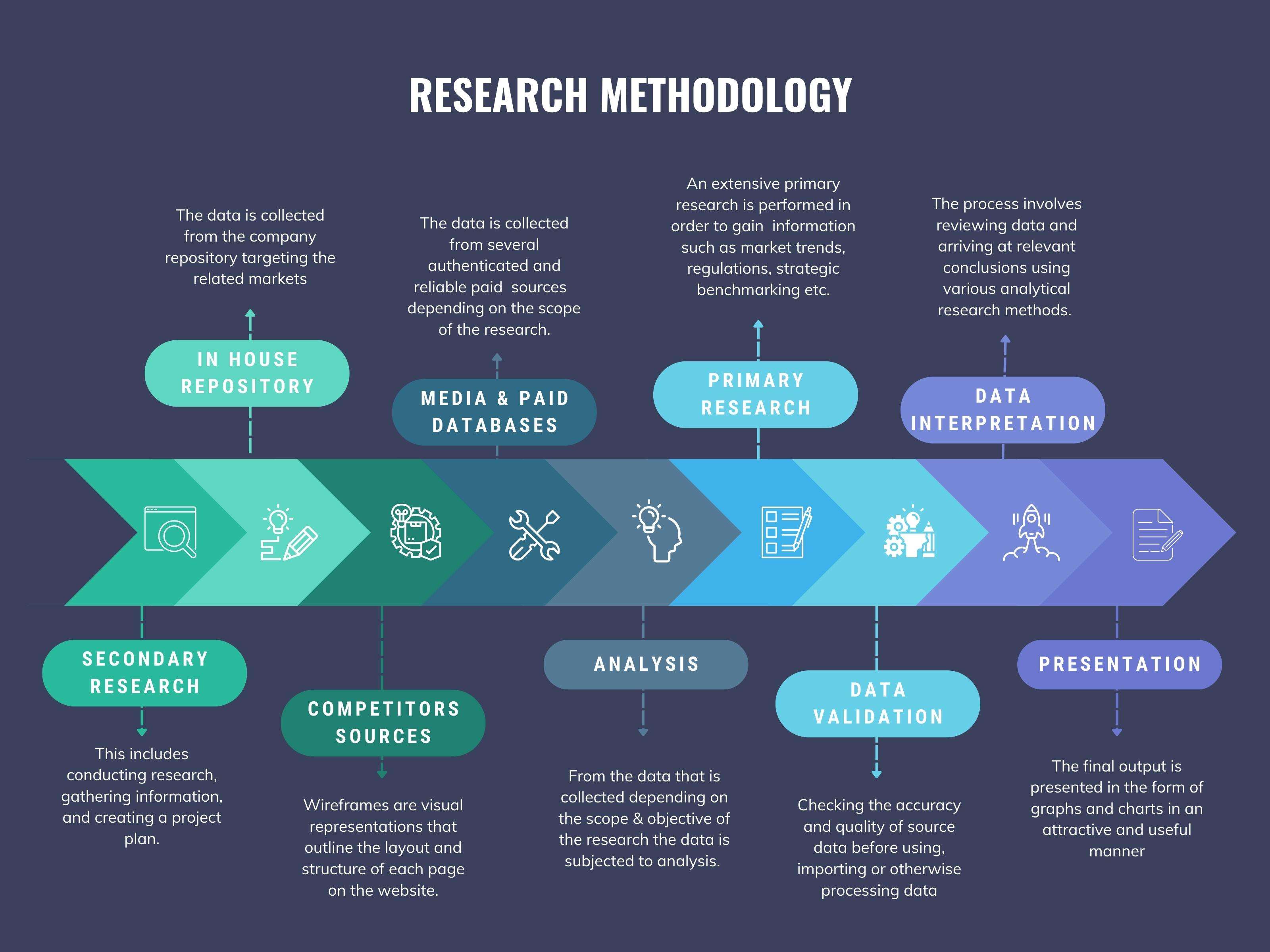
We at ‘Stratistics’ opt for an extensive research approach which involves data mining, data validation, and data analysis. The various research sources include in-house repository, secondary research, competitor’s sources, social media research, client internal data, and primary research.
Our team of analysts prefers the most reliable and authenticated data sources in order to perform the comprehensive literature search. With access to most of the authenticated data bases our team highly considers the best mix of information through various sources to obtain extensive and accurate analysis.
Each report takes an average time of a month and a team of 4 industry analysts. The time may vary depending on the scope and data availability of the desired market report. The various parameters used in the market assessment are standardized in order to enhance the data accuracy.
Data Mining
The data is collected from several authenticated, reliable, paid and unpaid sources and is filtered depending on the scope & objective of the research. Our reports repository acts as an added advantage in this procedure. Data gathering from the raw material suppliers, distributors and the manufacturers is performed on a regular basis, this helps in the comprehensive understanding of the products value chain. Apart from the above mentioned sources the data is also collected from the industry consultants to ensure the objective of the study is in the right direction.
Market trends such as technological advancements, regulatory affairs, market dynamics (Drivers, Restraints, Opportunities and Challenges) are obtained from scientific journals, market related national & international associations and organizations.
Data Analysis
From the data that is collected depending on the scope & objective of the research the data is subjected for the analysis. The critical steps that we follow for the data analysis include:
- Product Lifecycle Analysis
- Competitor analysis
- Risk analysis
- Porters Analysis
- PESTEL Analysis
- SWOT Analysis
The data engineering is performed by the core industry experts considering both the Marketing Mix Modeling and the Demand Forecasting. The marketing mix modeling makes use of multiple-regression techniques to predict the optimal mix of marketing variables. Regression factor is based on a number of variables and how they relate to an outcome such as sales or profits.
Data Validation
The data validation is performed by the exhaustive primary research from the expert interviews. This includes telephonic interviews, focus groups, face to face interviews, and questionnaires to validate our research from all aspects. The industry experts we approach come from the leading firms, involved in the supply chain ranging from the suppliers, distributors to the manufacturers and consumers so as to ensure an unbiased analysis.
We are in touch with more than 15,000 industry experts with the right mix of consultants, CEO's, presidents, vice presidents, managers, experts from both supply side and demand side, executives and so on.
The data validation involves the primary research from the industry experts belonging to:
- Leading Companies
- Suppliers & Distributors
- Manufacturers
- Consumers
- Industry/Strategic Consultants
Apart from the data validation the primary research also helps in performing the fill gap research, i.e. providing solutions for the unmet needs of the research which helps in enhancing the reports quality.
For more details about research methodology, kindly write to us at info@strategymrc.com
Frequently Asked Questions
In case of any queries regarding this report, you can contact the customer service by filing the “Inquiry Before Buy” form available on the right hand side. You may also contact us through email: info@strategymrc.com or phone: +1-301-202-5929
Yes, the samples are available for all the published reports. You can request them by filling the “Request Sample” option available in this page.
Yes, you can request a sample with your specific requirements. All the customized samples will be provided as per the requirement with the real data masked.
All our reports are available in Digital PDF format. In case if you require them in any other formats, such as PPT, Excel etc you can submit a request through “Inquiry Before Buy” form available on the right hand side. You may also contact us through email: info@strategymrc.com or phone: +1-301-202-5929
We offer a free 15% customization with every purchase. This requirement can be fulfilled for both pre and post sale. You may send your customization requirements through email at info@strategymrc.com or call us on +1-301-202-5929.
We have 3 different licensing options available in electronic format.
- Single User Licence: Allows one person, typically the buyer, to have access to the ordered product. The ordered product cannot be distributed to anyone else.
- 2-5 User Licence: Allows the ordered product to be shared among a maximum of 5 people within your organisation.
- Corporate License: Allows the product to be shared among all employees of your organisation regardless of their geographical location.
All our reports are typically be emailed to you as an attachment.
To order any available report you need to register on our website. The payment can be made either through CCAvenue or PayPal payments gateways which accept all international cards.
We extend our support to 6 months post sale. A post sale customization is also provided to cover your unmet needs in the report.
Request Customization
We offer complimentary customization of up to 15% with every purchase. To share your customization requirements, feel free to email us at info@strategymrc.com or call us on +1-301-202-5929. .
Please Note: Customization within the 15% threshold is entirely free of charge. If your request exceeds this limit, we will conduct a feasibility assessment. Following that, a detailed quote and timeline will be provided.
WHY CHOOSE US ?

Assured Quality
Best in class reports with high standard of research integrity

24X7 Research Support
Continuous support to ensure the best customer experience.

Free Customization
Adding more values to your product of interest.

Safe & Secure Access
Providing a secured environment for all online transactions.

Trusted by 600+ Brands
Serving the most reputed brands across the world.
